Now that COVID-19 vaccines have reached billions of humans internationally, the proof is overwhelming that no matter which one you take, the vaccines provide lifestyles-saving protection in opposition to an ailment that has killed tens of millions. The pandemic is a long way from over, and they are our excellent guess of staying safe.
WHAT ARE THE DIFFERENT TYPES OF COVID-19 VACCINES?
There are four styles of vaccines in medical trials: complete virus, protein subunit, viral vector, and nucleic acid (RNA and DNA), each of which protects human beings, however, by using producing immunity in a barely distinctive way.
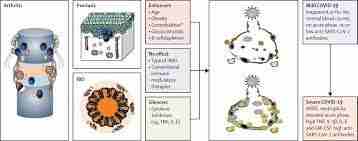
Abstract
Large-scale covid19 ailment 2019 (COVID-19) vaccination programs were rolled out internationally. Vaccines that might be broadly used globally encompass mRNA vaccines, adenoviral vector vaccines, and inactivated whole-virus vaccines. COVID-19 vaccines can result in various facet outcomes. Among the maximum common of these unfavorable consequences are pain at the injection site, fatigue, and headaches. Some facet effects must be more well documented, including joint-related adverse effects. In this evaluation, we determine the epidemiology and medical features of published COVID-19 vaccination joint-related destructive results based on the assessment of sixteen affected person case reviews.
Based on our evaluation, we located that females formed the majority of the instances, accounting for 62.5% of patients, while 37.5% of the cases were men. The mean age of presentation of the various patients changed to 54.8 years, with a preferred deviation (SD) of 17.49 years. In 37.5% of the cases, patients received the Sinovac vaccine. The proportion of patients who acquired different vaccines became as follows: the Pfizer vaccine: 31.25%; Sputnik V: 12.5%; Moderna, AstraZeneca, and Covaxin: 6.25% every.
Discussion
Vaccinations are the primary device in preventing infectious illnesses. However, neighborhood, systemic, and autoimmune (autoimmune/inflammatory syndrome induced employing adjuvants [ASIA syndrome]) side results had been reported related to vaccinations. It is an idea that vaccinations can trigger or expand autoimmunity, even though the effect mechanism is only sometimes ultimately acknowledged [5]. This could be due to the immunogenic content (inactivated virus) or adjuvants located inside the vaccination. Therefore, at the same time as vaccines prevent the improvement of autoimmune illnesses brought about by infections, autoimmunity can also be prompted after vaccination.
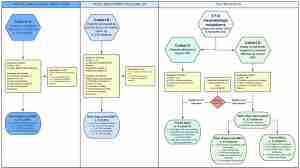
The COVID-19 Vaccine and Your Bones and Joints
Many orthopedic sufferers have questions about how the COVID-19 vaccine could impact their bones and joints.
The American Academy of Orthopaedic Surgeons (AAOS) has stated that the blessings of the COVID-19 vaccine strongly outweigh the orthopedic risks. AAOS offers its complete help for the massive adoption of the vaccine.
This valuable resource was created to assist cope with issues you can have approximately the impact of the COVID-19 vaccine on your musculoskeletal fitness. Don’t hesitate to contact your orthopedic medical professional if you have any questions or need extra data.
Introduction

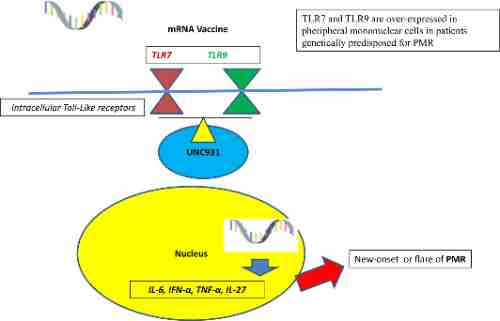
The coronavirus ailment 2019 (COVID-19) occasionally causes autoimmunity (1). Molecular mimicry has been considered a concern in improving autoimmunity because of the go-reactivity of a COVID-19 spike protein to human antigens (1). Given that BNT162b2 (BioNTech-Pfizer) is an mRNA-primarily based vaccine expressing the spike protein, it’s far possible that BNT162b2 vaccination can be a cause for the development of autoimmunity (2–four). In reality, new-onset or flares of autoimmune problems, including rheumatoid arthritis (RA), person-onset Still’s disorder, inflammatory bowel diseases, and anti-neutrophil cytoplasmic antibody-associated vasculitis had been located quickly after the COVID-19 vaccination (5–9). Immunopathogenesis underlying COVID-19 vaccination-associated autoimmunity has no longer been fully understood. In this regard, sensing of double-stranded and single-stranded RNA derived from the mRNA-based vaccine via toll-like receptors (TLRs), retinoic acid-inducible gene-I (RIG-I), and cancer differentiation-related gene 5
(MDA5) may be potent triggers for the production of the kind I interferons (IFN-I) and pro-inflammatory mediators (2–four). Therefore, immoderate production of IFN-I and seasoned-inflammatory cytokines may be concerned with developing autoimmune responses related to COVID-19 vaccination.
Should people with arthritis get a vaccine?
It is critical for someone to get the COVID-19 vaccine if they’re medically capable of doing so.
2021 take, a look at The LancetTrusted Source notes that it’s far more beneficial for those with rheumatic illnesses to obtain the COVID-19 vaccination.
This is because the vaccine reducesTrusted Source the probability of contracting and spreading the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). It also helps save humans from developing an intense infection with COVID-19 if they settle the virus.
Additionally, people with certain medical situations have a higher riskTrusted Source of becoming severely unwell with COVID-19. This can boom the probability of:
- requiring hospitalization
- wanting in-depth care
- requiring a ventilator to help them breathe
- experiencing chronic signs, or lengthy COVID
- death
Are the vaccines safe for arthritis?
The COVID-19 vaccine is a safe and effective trusted Source, and a person with arthritis must get it if they’re medically capable of accomplishing that. However, in rare instances, it’s miles feasible that the vaccine can trigger an arthritis flare.
A 2021 look observed 1,519 humans with arthritis and other musculoskeletal conditions, such as RA, psoriatic arthritis, and different kinds of arthritis.
Of the contributors, seventy eight% acquired the Pfizer vaccine, 16% obtained the Oxford-AstraZeneca vaccine, 5% received the Moderna vaccine, and 1% received an uncertain vaccine type.